We may earn revenue from the products available on this page and participate in affiliate programs. Learn More ›
When Aaron Hipp’s left hand started to swell and grow hot, he knew his rash wasn’t getting better. When the skin began to blister into painful yellow pustules that seemed to be eating the flesh around his thumb, he knew he needed to go back to the doctor. He had seen a dermatologist for the rash a month earlier, but the cream he’d been prescribed seemed to be making things worse.
As the rash continued to spread, Hipp went for a second opinion. The new dermatologist took a big biopsy of his hand, and immediately discontinued Hipp’s initial medications. He had a fungal infection—not a bacterial infection, or even Lyme disease, as had been suggested. Once the doctors figured out was wrong with Hipp, they tried to figure out how he’d gotten the rash in the first place. Hipp is a lifelong hunter and angler, and he’s been a precision rifle competitor for the past 10-plus years. This is his story.
Some of you may call B.S., but for those who are willing to listen, my story could save you the misery I had to endure.
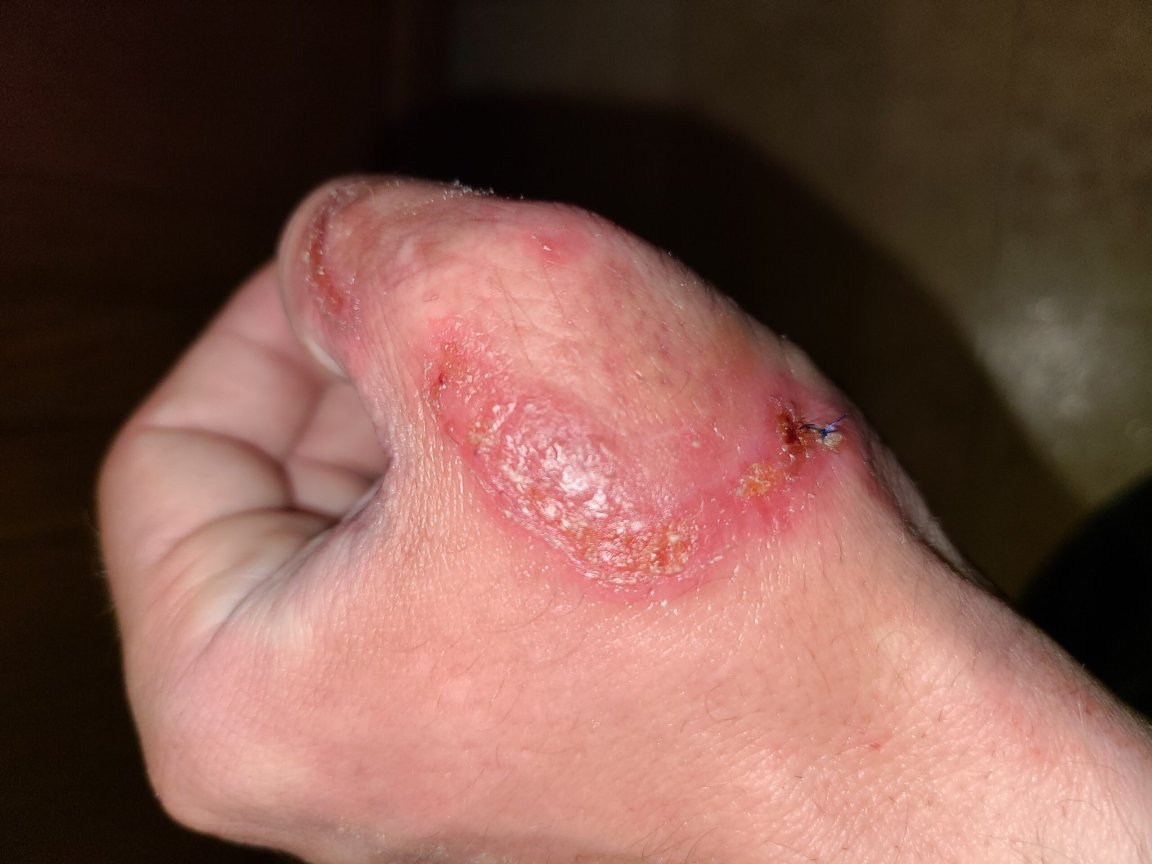
A couple months back, I started getting a rash on my left hand, on the back of my thumb and the meaty part. The first dermatologist I saw thought it was eczema and gave me a topical steroid (called clobetasol). But the rash continued to get worse, and it turned into a big open sore, like infected road rash. Pustules began to form. They would itch like mad while showing up, and then pop within about 24 hours…and then the open sore would continue to grow and spread. When the pustules popped, they would leave holes—open wounds that seemed to eat the flesh around them.

At one point, my doctor thought that perhaps I had gotten Lyme disease from a tick bite, and had put me on antibiotics for that. Luckily, my bloodwork came back negative for Lyme. A couple weeks after that, when the pustules were showing up again, I was lucky enough to get an emergency appointment at OSU dermatology. They biopsied my skin while the pustules were still present using a 5mm hole punch.
The doctor and I discussed my outdoor activities. The physicians mentioned that they had seen some interesting bacterial infections from hunters and anglers, and they put me back on another heavy dose of antibiotics while we were waiting on the biopsy results. When the biopsy results came back, they realized I didn’t have a bacterial infection, but a nasty fungal infection. They immediately took me off the antibiotics and topical steroids. It turns out topical steroids can make some fungal infections worse (which is what was happening with the clobetasol that the first dermatologist gave me).

But none of us knew how I had gotten the fungal infection. As we tried to figure out where I might have contracted the infection, the doctor told me to go through photos on my phone to see if I could determine when the rash appeared. As I looked through the photos on my phone, I realized that the rash showed up about a week and a half after the last coyote I had shot. I remember that coyote hadn’t been the healthiest looking, but nothing had seemed off about it. I also take a minimum precaution of dragging coyotes with my left hand, in case I end up eating or drinking something with my right hand while I’m out.
That timeline aligns with the lifecycle of some fungal infections, and the experts suspected I might have had an open cut on my hand that allowed the fungus to infect my hand. Think ringworm—but hopped up on serious drugs. And now I’m hopped on serious drugs, too. I’m on a 90-day cycle of oral antifungal pills, and I may have to take other medication if this doesn’t work completely. It does appear to be working so far, but oral antifungals are hard on your liver and they can have some not-so-fun side effects.
I’m sure my fungal infection from dragging a coyote was one of those one-in-one-thousand events. But let me tell you that it was a nasty experience that ate my hand up, and I never want to get it again. I have no plans to stop hunting, but I’ll definitely be wearing nitrile gloves 100 percent of the time when dealing with any animals while hunting.
When I shared my story on some hunting forums, I heard from a number of other hunters who had contracted a fungal or bacterial infection on a hunting or fishing trip. Some guys mentioned they had been on medication for over a year to clear up what they caught. A lot of people shared their home remedies in response to my post, too. It’s interesting because if you look up what some people recommend, you can quickly confirm they would be useless when compared to medical literature and could even make things worse if you apply the solution to the wrong situation.

What are the takeaways for me?
– As hunters, do we get too comfortable seeing a sick coyote, and just call it mange when it’s something else that could be way worse—and transferable to us? The coyote I dealt with didn’t give me any concerns, yet here I am. We should probably be more cautious with the animals we handle. Animals can get fungal and bacterial infections that may be mild for them, and worse for us.
– Stand up for your health early. We probably disregard infections and rashes more often than we should. Know when it’s time to see a doctor, and if things don’t get better, don’t be afraid to see a different doctor. Ask for bloodwork, and for biopsies. If there is a test that can confirm or eliminate possibilities, there’s no reason not to have it performed. You are responsible for your health, and not all doctors are equally competent.
– Be very careful with home remedies. Some may help, some may do nothing, others may make things worse and potentially cause other health issues.
– Take pictures. I took pictures when the rash started showing up for my own purposes to see if it was getting better or worse. These pictures and timeline were helpful to the dermatologists I saw laster, so they could better determine potential causes and make a diagnosis. Dermatology issues are notoriously difficult to diagnose.
– Don’t stop hunting, but take precautions. I generally hunt coyotes at night using thermal and night vision. It’s amazing how peaceful it is being out in the middle of a field in pure darkness, yet you can see everything going on around you. Deer will walk within 30 feet of you, and never know you are there. I’ve watched families of foxes play for what seemed like an hour and had racoons and other animals almost run across my feet and owls almost take the hat off my head. It’s a completely different experience at night interacting with the wildlife. I’m just going to be wearing gloves from now on whenever I touch or clean an animal.
Anyone else ever caught anything from an animal they killed?
Sincerely,
Aaron Hipp
Aaron Hipp owns Kinetic Security Solutions, which makes the Adaptive Tuning System for precision shooting and hunting applications. He enjoys coyote hunting because it uses many of the same techniques and skills required in rifle competitions, such as positional shooting from tripods and shots on moving targets.
Common Fungal Infections Hunters Can Get from Game
While the risk of fungal infection from the game we hunt is relatively low, it’s not impossible to contract something nasty, like in Hipp’s case. There are five main types of fungal infections that hunters are most likely to get: Blastomycosis, coccidioidomycosis (also known as desert or valley fever), Cryptococcus gattii, histoplasmosis, and ringworm. Except ringworm, each of these fungal infections is caused by inhalation of fungal spores.
Blastomycosis
This fungal infection is found in the eastern half of North America, usually in moist soil and decomposing leaves and organic matter, and along waterways. According to the Center for Disease Control and Prevention, people who participate in outdoor activities that expose them to wooded areas (such as forestry work, hunting, and camping) in these areas may be at higher risk for getting blastomycosis, although people with weakened immune systems are more likely to develop severe blastomycosis. The real concern with this fungal infection is that your dog is 10 times more likely to get it than you are, given that dogs tend to disturb soil more than humans. Blastomycosis cannot spread between people or between people and animals, which means your dog and the game you hunt.

Valley Fever
Valley fever occurs the same way Blastomycosis does—when you inhale fungal spores. The fungus that causes valley fever, Coccidioides, lives in in Arizona, California, Nevada, New Mexico, Texas, and Utah, and it was also recently found in south-central Washington, according to the CDC. Again, your dog appears more likely to contract this fungal infection than you, but cannot give it to you. During dry spells, the mold goes dormant in the soil, where it can remain dormant for prolonged periods of time, according to Krista Williams of the VCA. “Once the rains come, the fungus grows and produces long filaments of mold that contain infectious spores. The tiny spores readily become airborne when the soil is disturbed by winds or by construction, farming, or digging.”

C. Gatti Infection
Cryptococcus gattii is a fungus that is found across the globe and much like the previous two fungi, it is found in the soil—specifically the soil around trees, as well as on trees and in tree hollows. While C. gattii primarily lives in tropical and subtropical areas of the world, it can be found on the mainland of British Columbia, Vancouver Island, Oregon, Washington, and California. This is a pretty rare infection that’s more likely to affect people with a weakened immune system, as well as people who smoke and are older than 50.
Histoplasmosis
The last of the main soil-based fungal infections hunters should know about is histoplasmosis. The fungus is most often found in soil that contains lots of bat and bird droppings, which in the U.S. mostly means central and eastern states, especially areas around the Ohio and Mississippi River valleys. “People can get histoplasmosis after breathing in the microscopic fungal spores from the air,” according to the CDC. “Although most people who breathe in the spores don’t get sick, those who do may have a fever, cough, and fatigue. Many people who get histoplasmosis will get better on their own without medication, but in some people, such as those who have weakened immune systems, the infection can become severe.” To reduce your likelihood of contracting histoplasmosis, people with weakened immune systems should avoid digging in soil or chopping wood where there are bird or bat droppings, as well as cleaning chicken coops or exploring caves you stumble across.

Ringworm
But the most common fungal infection in humans is ringworm. Ringworm is a general name for a fungal infection that’s caused by many types of fungi, and it’s behind everything from athlete’s foot to jock itch. The disease gets it name from the appearance of a ring-like rash that develops on the skin of the infected person or animal. (Despite the name, the disease has nothing to do with worm.) These fungi are present in the soil, on humans, and animals, and certain conditions can lead to an infection. You can contract ringworm from direct contact with another person or an animal that has it, as Hipp did when he touched the coyote. Again, your dog can get ringworm, as can cats, horses, rabbits, goats, and more livestock. It’s been documented in deer in Alberta, as well as in wild carnivores. It’s not always obvious if a wild animal has it, but you can identify ringworm as scaly round areas of hair loss, which explains why some ringworm-infected coyotes could be mistaken as having mange. (In some cases, as with this California black bear cub, it’s possible for an animal to have both.)
Regular showers after handling wild animals, as well as baths after hunting trips for your four-legged hunting buddy, are important. Symptoms of ringworm in dogs—including hair loss, red, dark, or blotchy skin and itchiness—should all be handled swiftly and properly by a veterinarian. Fungal infections aren’t a common issue in the hunting world, but when they do arise—as in Hipp’s case—it’s important to handle the situation appropriately and swiftly.

Other Common Infections Hunters Can Get
It will come as no surprise to many of you that fungal infections tend to be the exception in the outdoors, rather than the norm. Part of this is because kicking up soil and inhaling fungi spores isn’t all that common when you’re sitting up in your treestand or bushwhacking for grouse. Bacterial and parasitic infections from consuming game meat is a concern, as well as diseases from ticks and other insects. For a full list of diseases that hunters and their dogs can get from animals, you can check out this list from the American Veterinary Medical Association and this list of wildlife-related diseases from the CDC. This field guide to common wildlife diseases and parasites in the Northwest Territories is also helpful, even if all the species covered don’t apply to you. We’ve highlighted some of the more common diseases and infections below, but it’s also smart to be aware of diseases like hantavirus (spread by rodents), the West Nile virus (contagious through the bites of infected mosquitoes), and rabies.
Brucellosis
Brucellosis is one of the main diseases of concern for hunters, according to the CDC. While it’s commonly known among feral hog hunters, brucellosis is a bacterial infection carried by many popular American game species and is therefore one of the more common diseases you’re likely to receive when handling animals. Deer, elk, bison, moose, and caribou are all likely to carry the bacteria, as well as predators such as bear and wolves who may feed on infected prey.
You can get sick if blood, fluid, or tissue from an infected animal comes in contact with your eyes, nose, mouth, or skin, which means you can get brucellosis while field dressing, butchering, handling raw meat, or eating undercooked meat of an infected animal. (And, like the fungal infections mentioned above, your dog can also contract this disease.) Signs and symptoms of brucellosis can include fever, chills, sweating, headache, low appetite, fatigue, and joint or muscle pain, and can occur anywhere from a week up to several months for you to start feeling sick. You can read more about brucellosis prevention for hunters and symptoms here.
Giardia
Giardia is the microscopic parasite that makes us all filter our water when we’re hunting or camping. It’s commonly contracted by drinking water contaminated by giardia-infected feces, such as in lakes and rivers. Sometimes people with giardia have no symptoms, but it can also cause gastrointestinal issues that begin 1 to 2 weeks after contacting the parasite.
Tick-Borne Illnesses, Like Lyme Disease
Tick-borne diseases are on the rise. Lyme disease gets the most attention, although it’s widely misdiagnosed, and there are a host of regional tick-borne disease that can affect hunters, including an alpha-gal allergy (aka the red-meat allergy), rocky mountain spotted fever, and scores more.
Trichinellosis
More commonly known as trichinosis, trichinellosis used to be associated with raw or undercooked pork, but now it’s more commonly contracted from wild game like bear. According to the CDC, “Trichinella parasites can infect a wide range of animals worldwide. In the lower 48 states, trichinellosis cases and outbreaks have been caused by the consumption of brown and black bear, wild boar, and cougar; in Alaska, walrus and black, brown, grizzly, and polar bear; and in Hawaii, wild boar. Trichinella has also been detected in many other wild animals that are hunted, including coyotes, foxes, and raccoons. Coyotes and foxes have not yet been implicated in any reported trichinellosis cases or outbreaks, but there has been at least one reported case attributed to the consumption of undercooked raccoon meat.”
People with trichinosis may initially experience gastrointestinal issues like diarrhea, stomach cramps, nausea, and vomiting, which are often followed by fever, muscle pains, facial swelling, and fatigue. These symptoms can last from weeks to months and can vary in severity from mild to severe. The best way to prevent trichinosis is to cook whole cuts and ground meat from these animals to an internal temperature of 160°F. Smoking, freezing, or curing game meat does not kill all Trichinella species, and low–temp smoking will not kill Trichinella, either.
Tuberculosis
TB is a lot less common than it used to be among humans, but there are some rare instances of hunters contracting tuberculosis from deer. The CDC published a report in 2017 about a Michigan deer hunter who caught bovine tuberculosis while hunting in an area where two other hunters had caught tuberculosis more than a decade previously.

The Bottom Line on Infections for Hunters
While we can’t always prevent these diseases, the good news is that they’re all treatable if they’re caught in time. And prevention for most of these diseases and infections is relatively simple. Talk with your doctors and specialists about your outdoor lifestyle and do your best to track when, where, and how you might have gotten sick. Good health starts with proper disease prevention, so get in the habit of washing your hunting clothes regularly. Use permethrin and wash your hands and body in warm water with soap. Wear gloves and cover as much skin as possible when handling game to avoid unnecessary contact with game meat and blood. Because the last thing any of us wants is to catch a preventable disease that keeps us out of the woods, so a little awareness and extra effort to keep yourself, your dog, and your gear clean goes a long way.